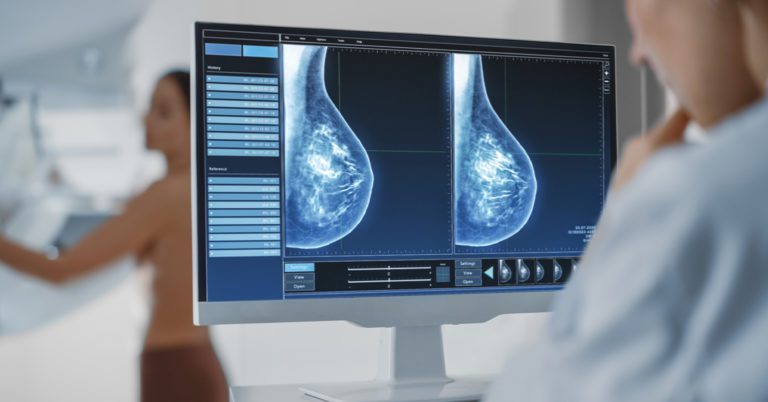
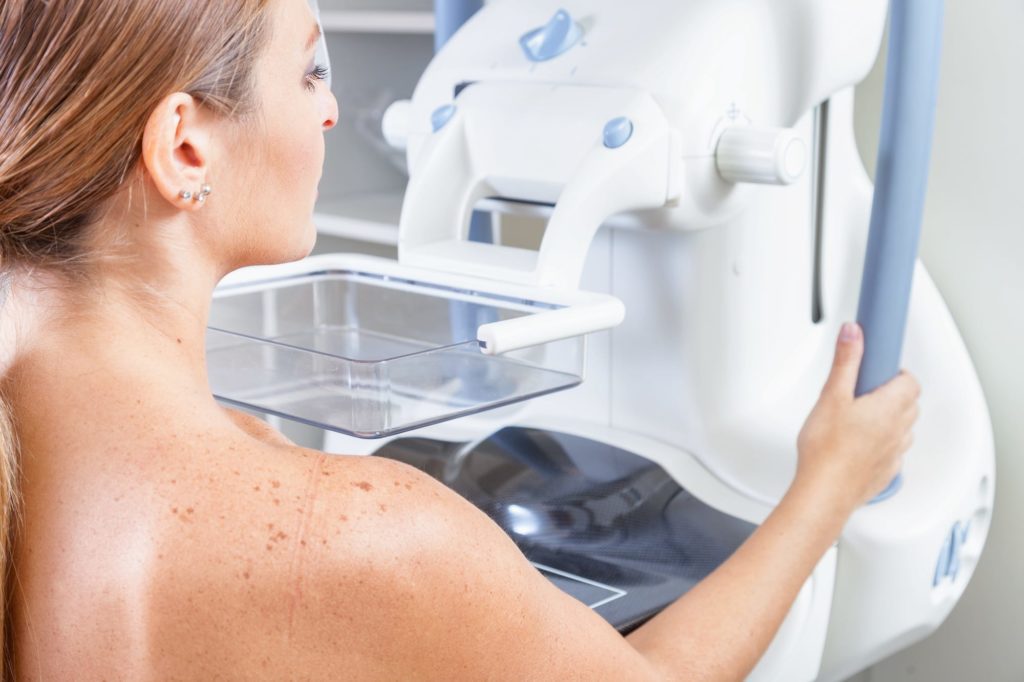
A screening mammogram takes approximately 20 minutes. We will provide a wrap or robe for you to change into prior to the test. During the test, the technologist will position your breasts to take images from multiple angles. Two views of each of breast are taken for a screening mammogram.
The breast compression portion of the mammogram lasts for a few brief seconds for each view.
A diagnostic mammogram requires more time than a screening mammogram. Your technologist takes a higher number of images so the radiologist can closely examine any areas of concern. Diagnostic mammogram appointments typically take 45 minutes to complete.
The following tips can help make your mammogram go smoothly.
TIME YOUR TEST.
Schedule your mammogram appointment after your period when your breasts will be less sensitive and/or swollen. This will help to minimize any discomfort and improve the quality of the images.
SHARE DETAILS.
The first time you visit Touchstone Medical Imaging for a mammogram, bring a list of important details about previous mammograms with you. Include dates and locations of those visits (if they were performed at another facility), as well as information about biopsies and treatments.
Tell the technologist performing your mammogram about any changes in your breasts or problem areas you have noticed. Describe any breast surgeries you have had, as well as your personal and family history of breast cancer. Also, let the technologist know if you are pregnant, breastfeeding or using hormone therapy.
Your technologist will ask questions about your COVID-19 vaccination history. Recent vaccination or boosters may cause the lymph nodes in your armpits to swell. This information is necessary for the radiologist interpreting your scan.
KNOW WHAT NOT TO WEAR.
Do not wear antiperspirant, deodorant or talcum powder to your appointment. These products can show up on your X-ray as white spots, which may resemble areas of abnormal breast tissue on the radiology images. Avoid one-piece outfits, such as a dress or jumpsuit. Instead, opt for a two-piece outfit so you only need to remove your shirt and bra for the mammogram.
Your doctor may have ordered a mammogram for a variety of reasons. A screening mammogram is recommended for any woman over the age of 40 or younger in those who are at high risk or have a family history of breast cancer. Additionally, if you have any concerns or unusual symptoms, including a breast lump, pain, or nipple discharge, a screening mammogram may be ordered to rule out breast cancer.
A diagnostic mammogram may be ordered if a screening mammogram was abnormal or inconclusive, or if you have a history of breast cancer. If you have had no previous symptoms, speak with your doctor about their recommendations or rationale for the mammogram they have ordered.
A mammogram should not hurt. Some women, especially those with sensitive breasts or nipples, may experience some minor discomfort when the breast tissue is pressed between the two plates. However, this discomfort should only last a few seconds and should be relieved as soon as the plates are no longer flattening the breast tissue.
A mammogram is a non-invasive diagnostic test that has been used for nearly 40 years. Some people debate whether a mammogram is necessary based on risk factors and weighing the risk versus benefits of radiation exposure. However, as we published in a prior post, the low-dose x-ray that is used in a mammogram is minimal. Others question whether mammograms are completely necessary based on the number of biopsies that are performed that return as benign (not harmful). However, mammograms are the only screening tool that has been proven to reduce breast cancer deaths. Since the 1990s when mammograms became standardized, the death rate has declined by 30%, and as we discussed in a previous post, the number of cases of detected breast cancer each year has doubled in the last decade, whereas the number of deaths has declined.
Consistent recommendations and advice span across the most relevant agencies and associations regarding mammograms. Current guidelines from the U.S. Department of Health and Human Services (HHS), the American Cancer Society (ACS), the American Medical Association (AMA), and the American College of Radiology (ACR) recommend screening mammography every year for women, beginning at age 40.
No! If you would like to have a screening mammogram done, you can make an appointment at any Touchstone Imaging location, or for a screening mammogram, we take walk-ins. However, because we are a medical imaging center and not a treatment facility, you do have to have a provider that we can send the results to — primary care, gynecologist, or family doctor are all fine.
According to the American Cancer Society, women should start considering annual mammograms beginning at 40 years old. If, however, you have a family history, including a parent or grandparent who has had breast cancer, it is recommended to get screenings beginning at the age they were diagnosed, or sooner for high-risk women.
For women aged 40 to 44, it is recommended to begin annual screening and strongly encouraged that women aged 45 to 54 make mammograms part of their annual routine. Women aged 55 and older can switch to a mammogram every other year unless they are high risk or have had a history of breast cancer.
Yes, mammograms are still recommended for women with breast implants. Although, you should let your technologist know that you have implants, what kind, and whether they are above or below the muscle. Because the mammogram may not fully penetrate the silicone or saline, additional images may be taken to ensure a complete picture is captured of the breast tissue. For women who have contractures (scar tissue), the mammogram may be uncomfortable, but the mammogram should not affect the implants.
Yes. Women’s imaging services are not a one-size-fits-all medical practice. For women who cannot have a mammogram or whose mammogram results have come back inconclusive, other options include a 3D mammogram, breast ultrasound, or breast MRI.
In the event there are abnormal results on one diagnostic imaging test, your provider may order another kind. Additionally, if you have a condition or have a previous history of mastectomy, a traditional mammogram may not be the best option. Discuss the options and risks versus benefits of each modality with your medical provider and radiology technologist.
Absolutely. At Touchstone Imaging, we staff women who are mammography-certified for this very reason. While all of our well-trained and high-skilled radiology technologists can perform a mammogram, all of our locations have women staff to keep our patients undergoing women’s imaging services comfortable.
Hormone changes during pregnancy can elevate your risk of breast cancer and exacerbate or encourage the growth of pre-existing breast cancer during pregnancy. Because of hormonal changes and milk production, detecting breast lumps may be more difficult. However, gestational breast cancer or pregnancy-associated breast cancer can develop quickly. If you discover a suspicious lump during your pregnancy, a mammogram is warranted.
Because a mammogram uses a low-radiation x-ray, routine or screening mammograms may be postponed if there are no signs or symptoms that would warrant it. However, if there are indications that you may have breast cancer, a mammogram should be performed right away. Because the radiation dose is so small and concentrated solely on the breast tissue, there is little to no risk to the baby. Because gestational breast cancer can be so aggressive, it is highly recommended that you do not wait until after delivery. However, if you or your medical provider are uncomfortable with a mammogram during your pregnancy, you can have an alternate procedure such as a breast ultrasound or breast MRI.
If you are breastfeeding, it may be difficult to get a clear image due to the full milk ducts. If you are scheduling a routine screening mammogram, it may be postponed until about three months after you are done breastfeeding. However, if you are experiencing any symptoms or lumps while breastfeeding, it is not recommended that you wait. The mammogram will not affect your milk or milk supply in any way, and you can immediately breastfeed once the mammogram is complete. We will ask that you breastfeed prior to the mammogram to empty the ducts as much as possible.
Yes! Because breast cancer can occur in men too, if you have any signs or symptoms that could indicate breast cancer, you may be referred for a mammogram. In fact, mammograms tend to be more accurate in men because the breast tissue is less dense. However, because a mammogram depends on pressing the breast tissue between two plates to flatten it, men who do not have enough breast tissue for this may be referred for alternative diagnostic imaging methods including breast ultrasound.