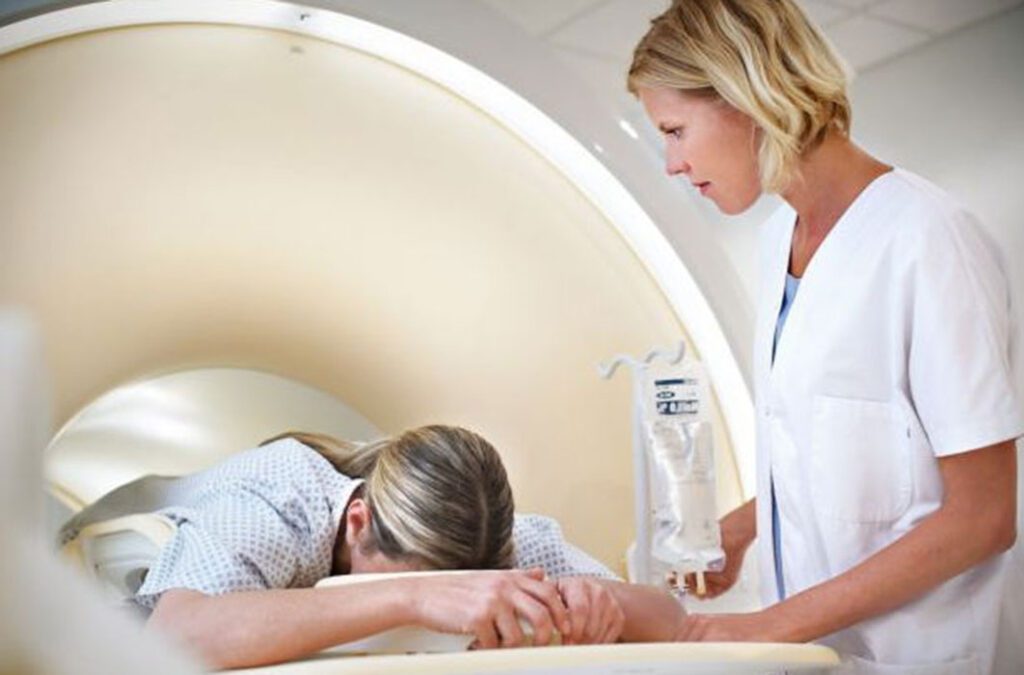
You will change into a gown and remove all jewelry and any other metal objects on you, as they interfere with the magnetic field of the MRI unit. You should not experience any discomfort during the exam because your breasts will not be compressed. If you suffer from claustrophobia or are anxious, you may want to ask your physician for a mild sedative. Please also notify our facility and your technologists at the time of your exam. We will walk you step by step through the process and exam to ease any fears you may have.
Most patients that are having this exam for diagnosis of breast cancer will receive a contrast injection during the exam. Sometimes contrast is not necessary if the study is to evaluate silicone breast implants. The scan will only take 15-20 minutes.
If you have had previous breast imaging at another facility besides Touchstone Medical Imaging, please bring the images and reports with you to your exam. Our radiologists need these for comparison purposes during the interpretation of your MRI.
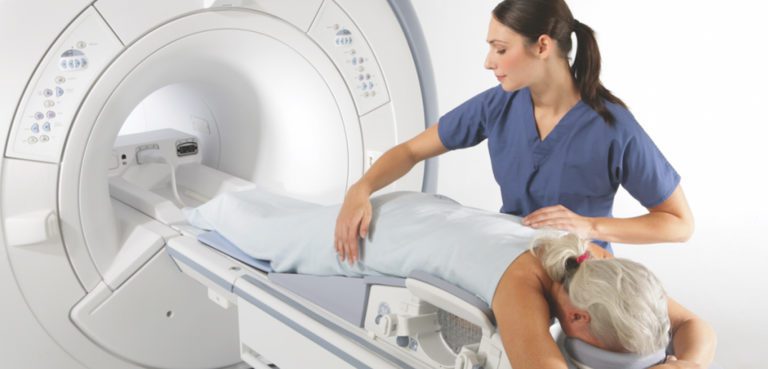
Breast MRI is just like any other MRI.
– We recommend that you wear comfortable, athletic-style clothing without metal snaps or zippers for the MRI.
– You may need to wear an exam gown during the study because snaps, zippers, hooks, belt buckles, and any other metal objects on your clothing affect the MRI.
– Complete your registration paperwork prior to your appointment.
– Prepare to arrive 20 minutes before your appointment time.
For women at high risk for breast cancer, typically because of a strong family history, an MRI may be an appropriate tool to screen for breast cancer. A strong family history is usually a mother or sister who has had breast cancer before age 50. It can also be aunts or cousins, including those on your father’s side. Relatives who have had ovarian cancer also increase your risk. Your radiologist or primary care doctor can look at your family history and determine if a breast screening MRI may be appropriate for you. Depending on your family history, genetic counseling may also be recommended.
After being diagnosed with breast cancer, a breast MRI may be performed to determine:
– How large the cancer is and whether it involves the underlying muscle.
If there are other cancers in the same breast and whether there is an unsuspected cancer in the opposite breast.
– If there are any abnormally large lymph nodes in the armpit, which can be a sign the cancer has spread to that site.
– Further evaluating hard-to-assess abnormalities seen on mammography
Sometimes an abnormality seen on a mammogram cannot be adequately evaluated by additional mammography and breast ultrasound alone. In these rare cases, MRI can be used to definitively determine if the abnormality needs biopsy or can safely be left alone.
Scarring and recurrent cancer can look identical on mammography and ultrasound. If there is a change in a lumpectomy scar by either mammography or on a physical exam, MRI can help determine whether the change is normal maturation of the scar or a recurrence of the cancer.
In some cases, breast cancer will be treated with chemotherapy before it has been removed by surgery. This is called neoadjuvant chemotherapy. In these cases, MRI is often used to monitor how well the chemotherapy is working and to reevaluate the amount of tumor still present before the surgery is performed.
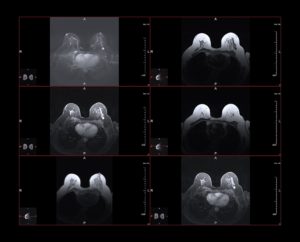
Yes, The FDA recommends an MRI as the best test for determining whether silicone implants have ruptured. Breast MRIs for implant evaluation require advanced equipment beyond the standard MRI machine. Please contact our locations to determine if this service is available near you.
Texas state legislation known as Henda’s Law requires mammography facilities to notify you and your health care provider if your results indicate dense breast tissue. As of September 2021, insurance regulations changed, which could cover the cost of your supplementary breast MRI exam.
Touchstone Medical Imaging provides breast MRI scans in the Dallas Fort Worth area at Downtown Fort Worth, Keller, Lewisville, Midlothian-Midway, and Red Oak.